Sharing Mayo Clinic
April 10, 2024
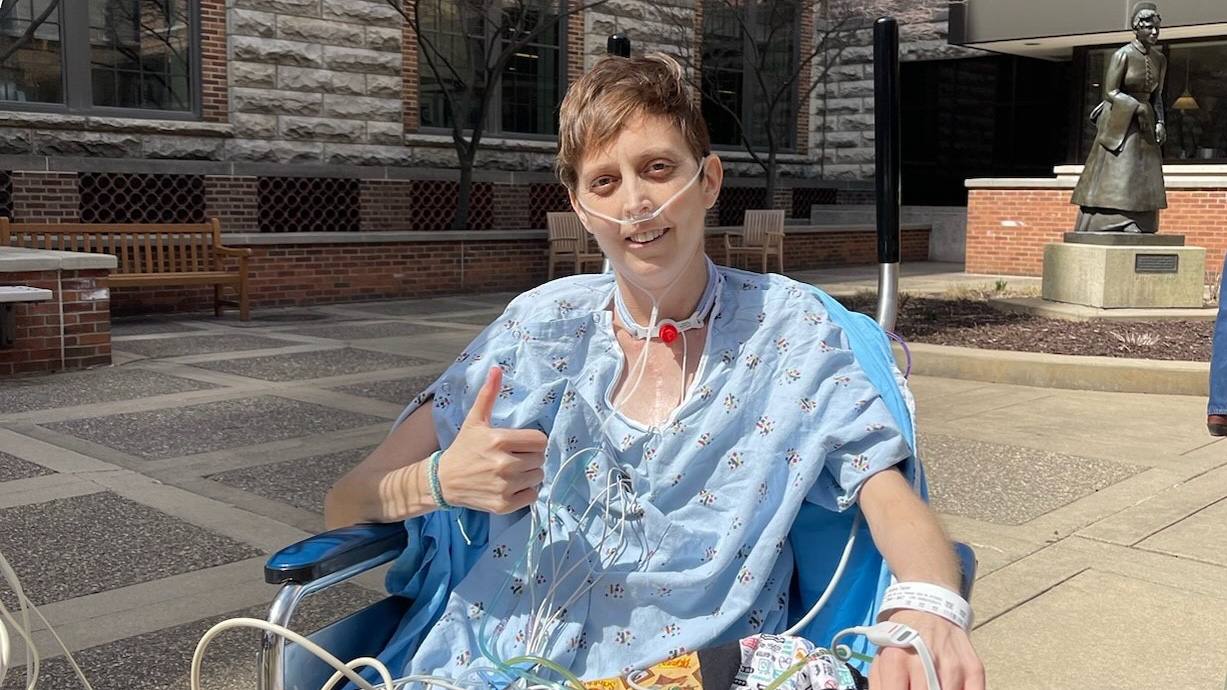
Britiny Schultz can't wait for fall. A huge football fan, she's looking forward to cheering on her favorite teams. It's something many fans take for[...]

March 25, 2024
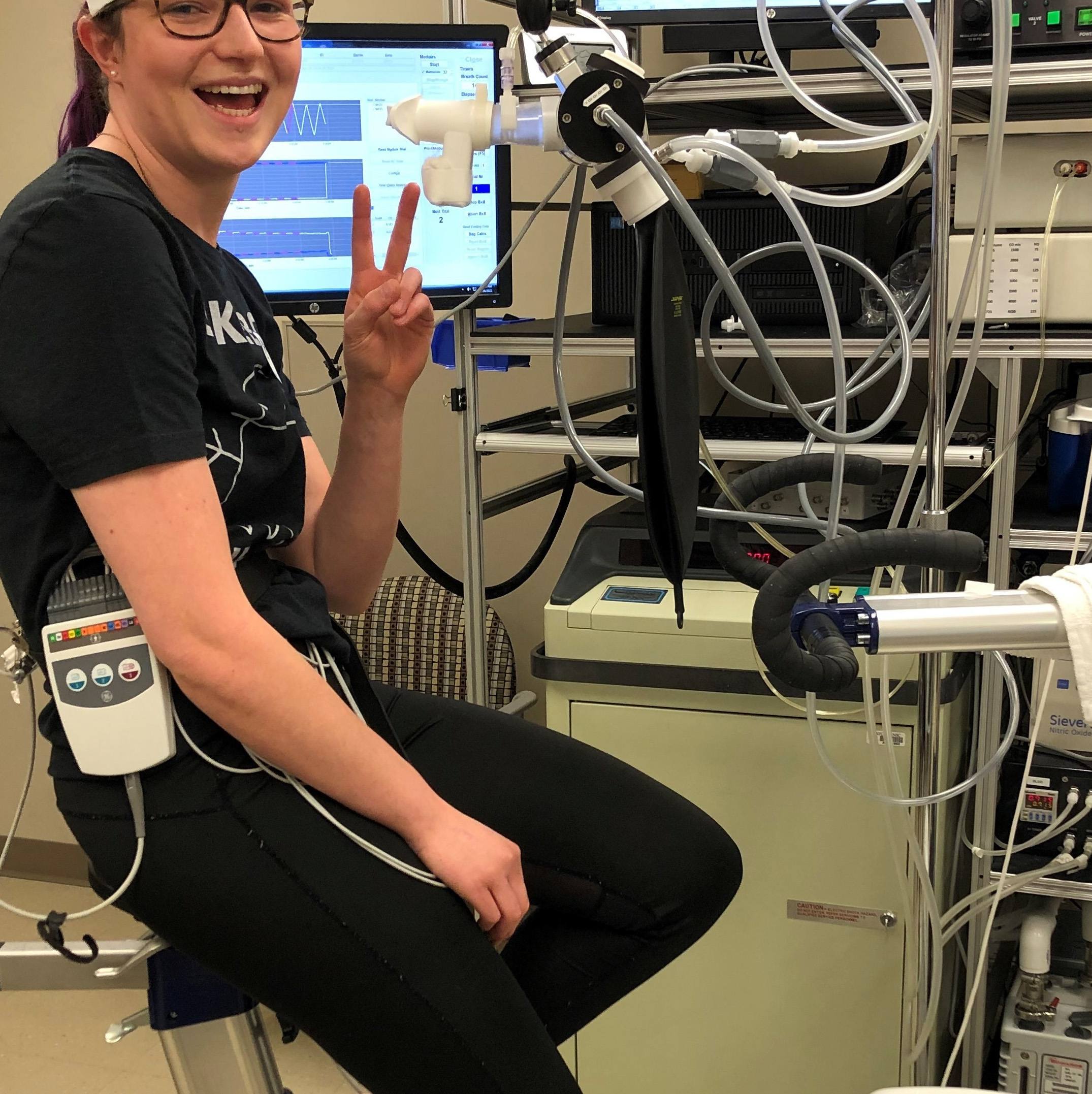
March 17, 2024

March 3, 2024

February 29, 2024
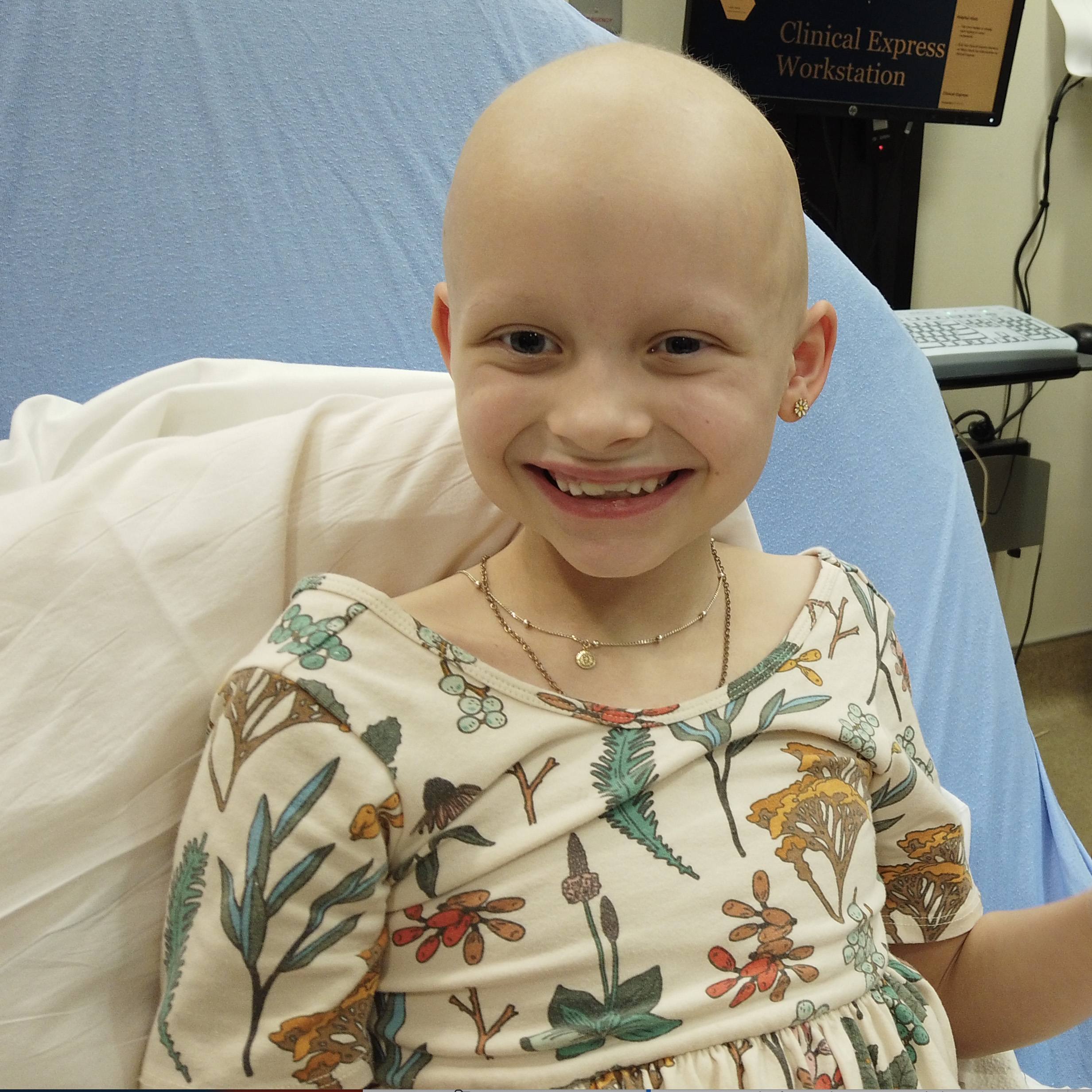
February 26, 2024

February 13, 2024

January 20, 2024
Explore more topics
 Sign up
Sign up

Mayo Clinic Connect
An online patient support community





