Sharing Mayo Clinic

May 16, 2024
Normally, hearing about a senior with hip problems would not be very surprising. But the senior you're about to meet is a senior in high[...]
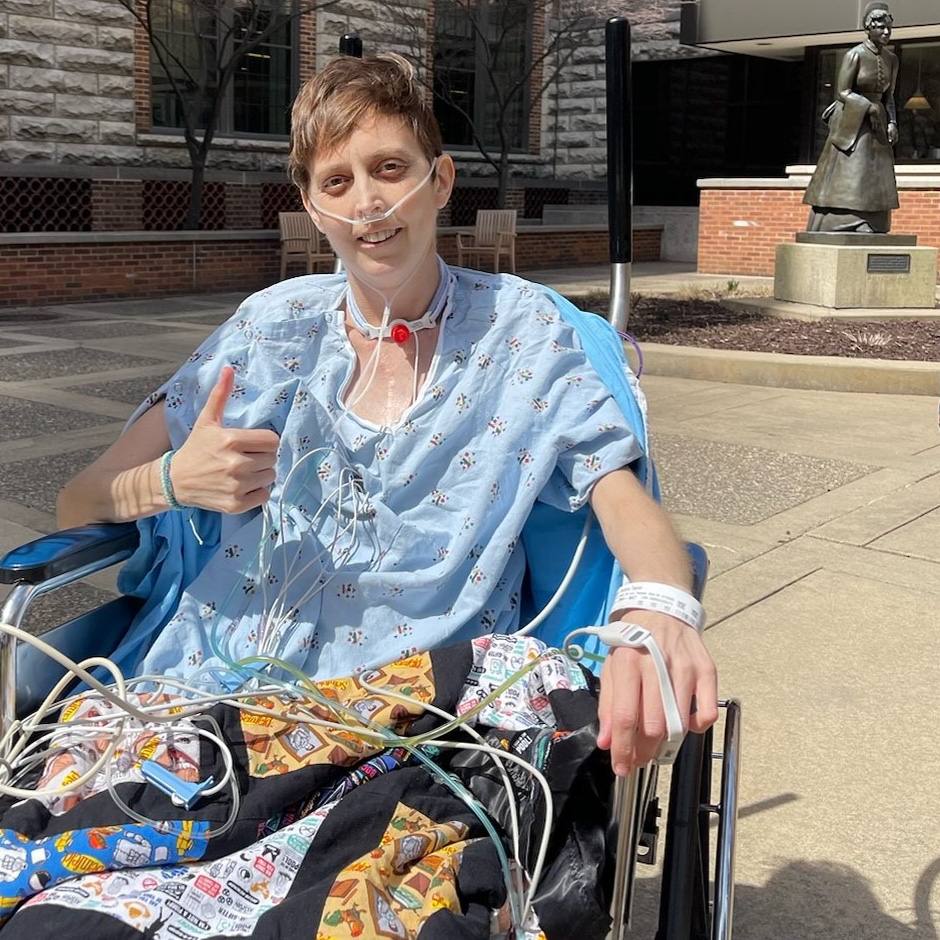
April 10, 2024

April 2, 2024

March 25, 2024
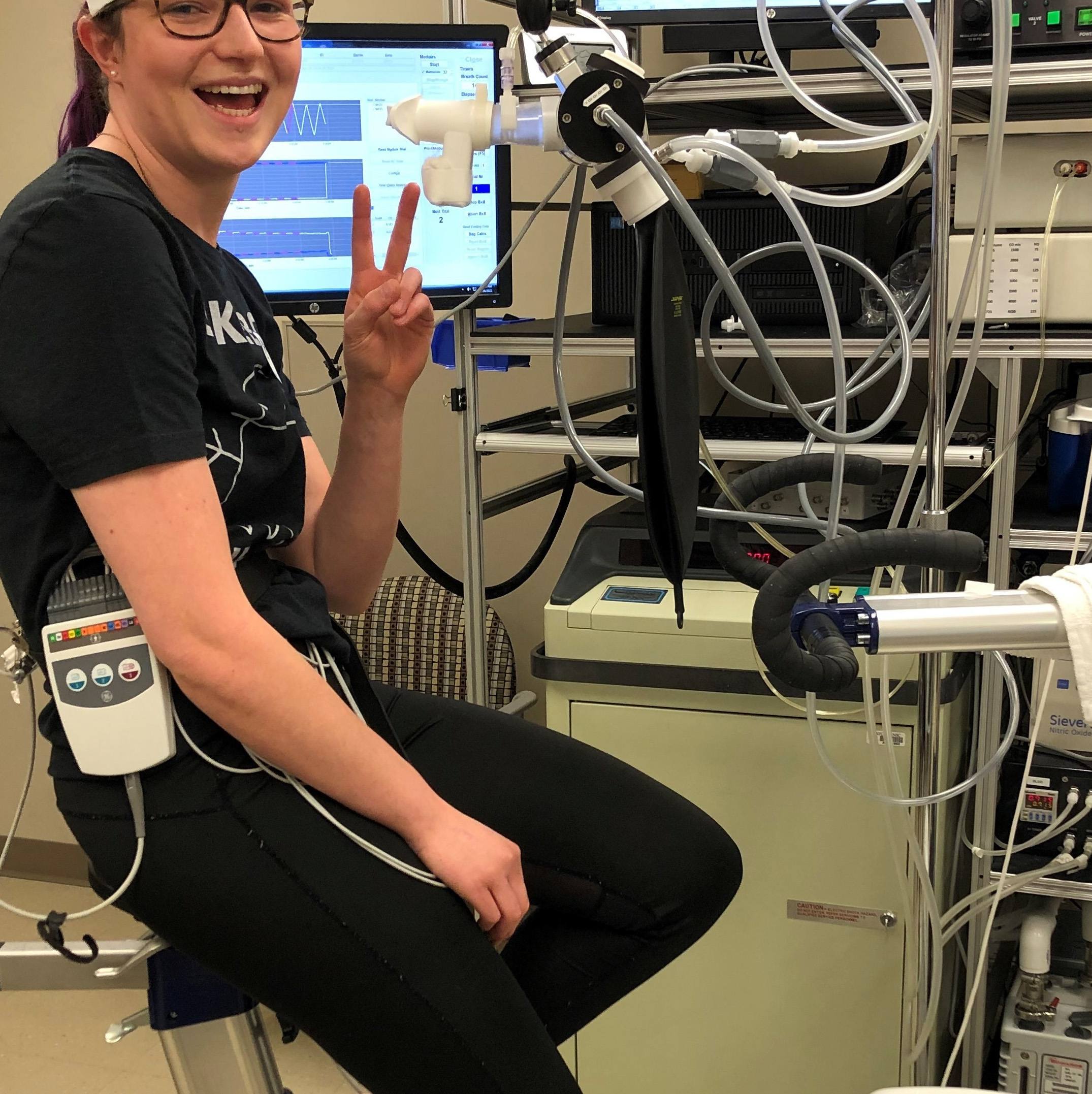
March 17, 2024

March 3, 2024

February 29, 2024
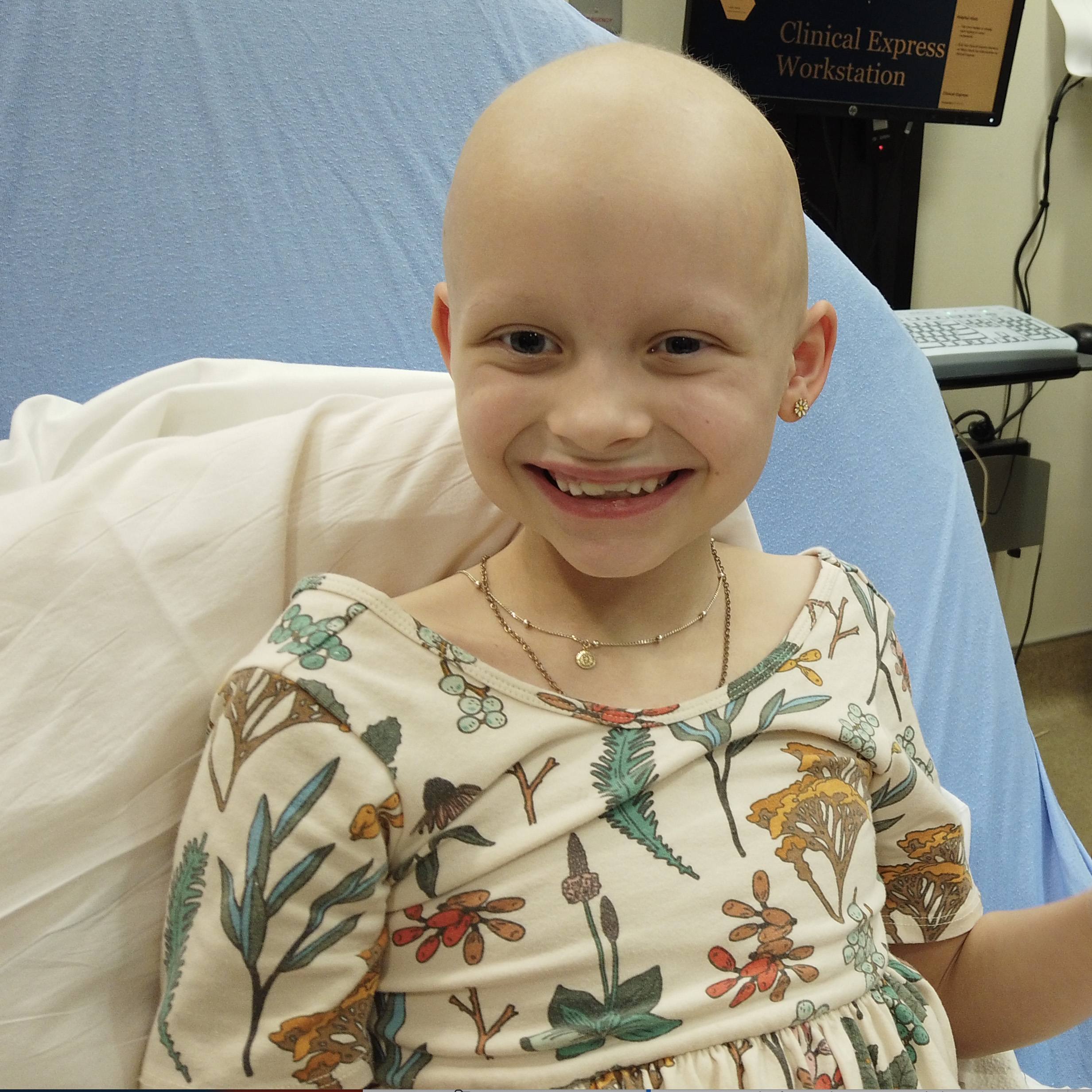
February 26, 2024
Explore more topics
 Sign up
Sign up

Mayo Clinic Connect
An online patient support community





